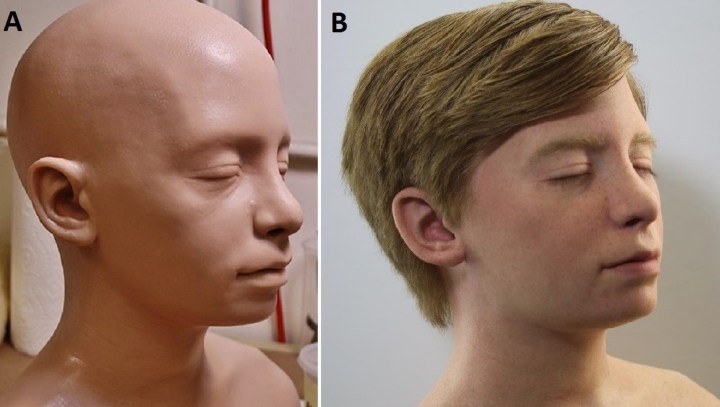
That’s our summary of recent work by a team of researchers from Johns Hopkins University School of Medicine. The model may be seem creepy, but it’s already offering trainees a realistic test subject.
“The model is highly accurate,” Alan Cohen, a professor of neurosurgery at Johns Hopkins who lead the project, told Digital Trends. “It is even more accurate than cadavers, because the model is based on MR (magnetic resonance) imaging from a real patient with the disorder being simulated, whereas cadavers do not usually have the pathologic disorders being taught.”
If available, minimally invasive neurosurgery is a procedure of choice for many surgeons because it doesn’t require a whole lot of poking and prodding. The operation is performed through tiny wholes using tiny instruments, with minimal brain trauma. However, tiny procedures don’t leave a whole lot of room for error and require some pretty sophisticated hand-eye coordination. As such, Cohen has dubbed the technique “Nintendo neurosurgery.”
“The procedure is done with miniaturized instruments inserted through working channels in an endoscope, a lighted tube similar to what the general surgeons used to take out the appendix or gall bladder in laparoscopic surgery,” he said. “The procedure is done with the surgical team guiding the instruments while watching a TV monitor.”
Though cadavers are the more conventional way to train medical students, they can be impractical. Each cadaver can only be used once, they’re relatively expensive, and hard to come by.
“Existing training methods are flawed,” Cohen said. “We sought to use 3D printing and a collaboration of neurosurgeons, neuroradiologists, simulation engineers, and a special effects team from Hollywood to create a novel training model for minimally invasive neurosurgery.”
The product of that collaboration — especially with special effects group FracturedFX — is a full-scale model that not only looks like a patient, but also has flowing cerebrospinal fluid and a realistically pulsating brain. In a study, neurosurgery fellows and medical residents performed surgery on the models and rated them highly for realism. Further tests will be needed to determine whether or not mock operations on the models improve operating room performance.
A paper detailing the study was published this week in the Journal of Neurosurgery.



