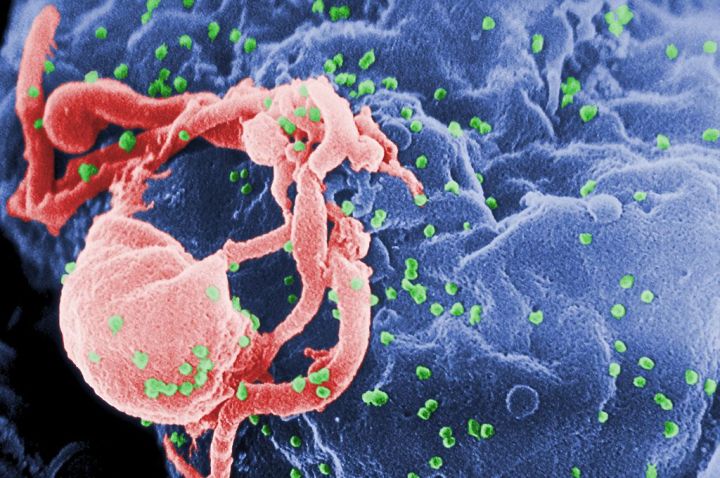
The CRISPR-Cas9 system is a popular gene-editing tool that is being used by multiple research groups in the fight against HIV. In one strategy, the CRISPR-Cas9 system was able to recognize the HIV in infected T cells and was further able to splice it out of the infected cell. According to a study published last week in the journal Cell Reports, this method appears to be effective at first, but select HIV survived the treatment and begin to infect T cells two weeks later. In these survival cases, DNA sequencing shows that the virus developed mutations near the section of DNA that was targeted by the CRISPR/Cas 9 system.
Researchers posit that these changes are not the result of random mutations, but instead are a byproduct of the Cas9 treatment itself. According to this theory, the mutations are introduced when the gene editing system cuts the DNA, and the cell tries to self-repair the excision, creating areas of DNA called indels. Some of these indels leave the HIV intact, allowing it to infect other T cells. This form of evasion is not surprising given how HIV works, but the speed at which it occurred was shocking to researchers.
Researchers believe these results are a manageable setback for the CRISPR/Cas9 method and intend to continue refining the treatment. Some researchers want to expand the gene editing technique to target multiple critical HIV genes while others propose a dual method of treatment that combined CRISPR gene editing with traditional antiretroviral HIV drugs to provide a double punch that’ll knock out the virus. Other proposed techniques to prevent HIV infection target the human heart’s T cells, seeking to make them resistant to infection. A clinical trial is currently underway to test this latter human-focused strategy using an alternative gene editing tool known as zinc-finger nucleases.
Editors' Recommendations
- Edit, undo: Temporary gene editing could help solve the mosquito problem
- Florida will release gene-edited mosquitoes into the wild, despite outcry
- CRISPR gene editing could help stop a common poultry virus in its tracks
- Scientists at UC San Francisco discover gene that helps supercharge sleep
- CRISPR gene editing to take on inherited blindness in U.S. study




